Knee Arthritis
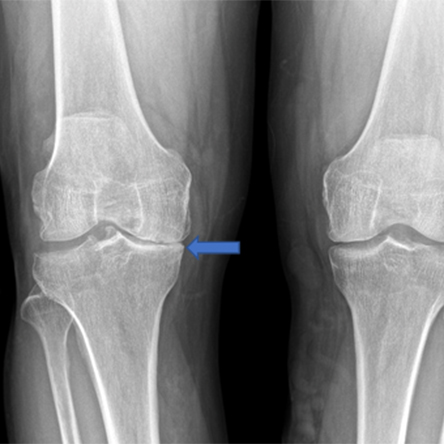
Arthritis is diagnosed by combining clinical symptoms (pain, stiffness, swelling, deformity) with radiographic (x-ray) findings (joint space loss, bone spur formation, cysts). Occasionally, patients will present with radiographic evidence of arthritis and have minimal clinical symptoms. Even if the x-rays show “bone-on-bone” arthritis, the treatment is always guided by the clinical symptoms and not the radiographic findings.
Hip Abductor Injury
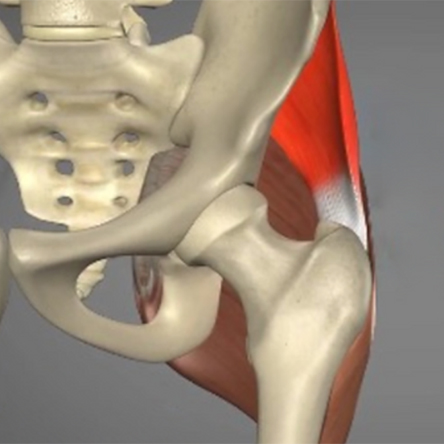
The hip abductors (comprised of the gluteus medius and gluteus minimus muscles) are often referred to as the “rotator cuff” of the hip. They function to abduct the hip and also to stabilize the pelvis while in single-leg stance (during running, jumping, pivoting, cutting or when going up and down the stairs…). Hip abductor tendon injuries or tears are diagnosed by combining clinical symptoms (pain, weakness) with MRI findings indicative of tendon degeneration, partial thickness tearing, or complete tearing. Hip abductor tendon injuries are different from muscle injuries and are divided into two types: acute and chronic.
Hamstring Tears
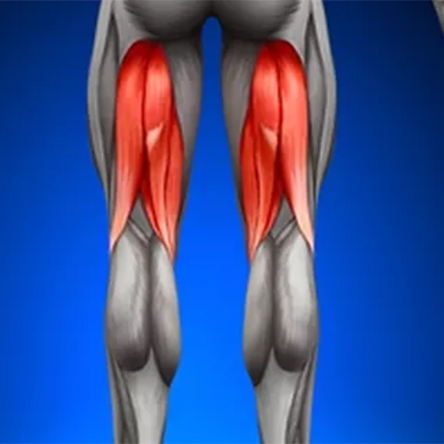
The hamstrings include three separate muscles (semitendinosus, semimembranosus and biceps femoris) that run along the back of the hip and knee joints. Collectively, they function to extend the hip and flex the knee during activities such as running and jumping. They originate on a part of the pelvis called the ischial tuberosity, a prominence that can be felt as the bony part of the buttock when you sit down on a hard surface. Hamstring injuries or tears are diagnosed by combining the patient’s story of an acute or chronic injury and clinical symptoms (pain, weakness, deformity) with MRI findings indicative of tendon degeneration, partial thickness tearing, or complete tearing.
Cartilage Damage
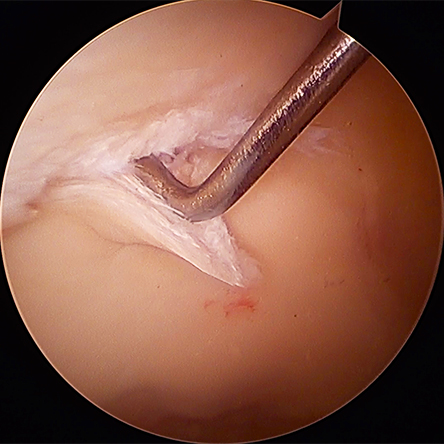
The hip is a synovial joint that is lined with smooth articular (surface) cartilage that also functions as a shock absorber. The joint is further lubricated with synovial fluid (joint fluid) creating a low friction environment for the femur (ball) to rotate and glide within the acetabulum (socket). Depending on the type of activity, forces transmitted across the hip joint can be several times the entire body weight of a person, placing significant load on the cartilage. Healthy cartilage is able to withstand these loads through numerous adaptations. There are two types of cartilage damage in the hip: focal, which is common in FAI and hip dysplasia, and generalized, which corresponds more with hip osteoarthritis (OA).
Hip Arthritis
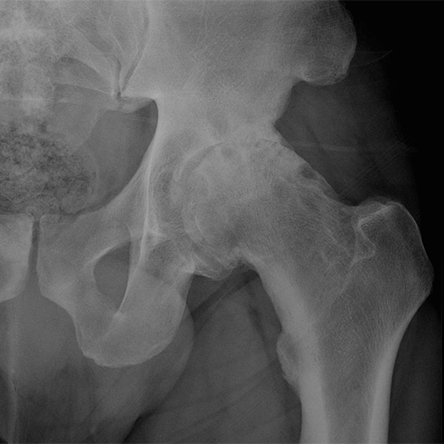
When cartilage damage to the hip is extensive and there is not enough cartilage in the hip to allow for consistent pain free weight bearing, the hip joint may not be salvageable. In this case, a hip replacement surgery may be the best treatment option to allow for improved function and decreased hip pain.
Trochanteric Bursitis
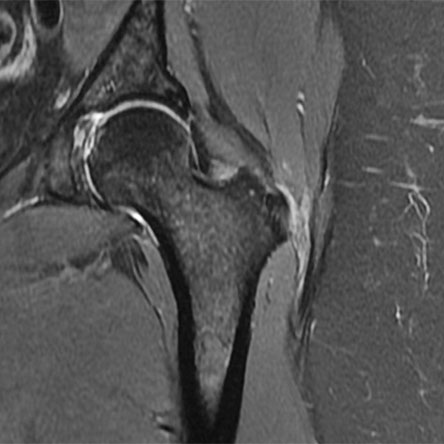
Trochanteric bursitis refers to an inflammation of the trochanteric bursa that typically develops over several weeks to months, causing pain and dysfunction. The condition is correlated with low back pain and degenerative disc disorders of the lumbar spine as well as with pelvic injuries and surgeries. As the lumbar and pelvic muscles become deconditioned, excessive stress is placed on the hip abductors, which are overloaded and cannot maintain proper pelvic balance during walking or standing. As a result, the loss of pelvic balance places excessive stress on the IT (ilio-tibial) band, which becomes tight and rubs on the greater trochanter. The increased pressure causes inflammation and thickening of the trochanteric bursa (bursitis), ultimately leading to pain and dysfunction and subsequently, if not treated promptly, to gluteus tendon tears.
Hip Impingement
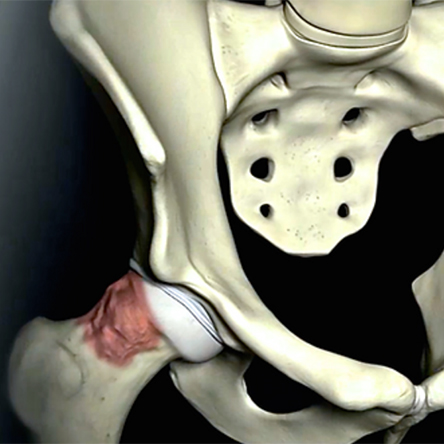
The term femoroacetabular impingement (or FAI) refers to a condition in which movement of the hip joint is restricted due to abnormal bony contact between the ball and hip socket. A common cause of FAI is a developmental abnormality of the ball resulting in bony overgrowth (cam lesion), which abuts against the rim of the socket during hip flexion and internal rotation. Alternatively, FAI may come about due to an excessively deep or abnormally oriented socket (pincer lesion) with a similar painful restriction in motion. Sometimes, the bony abnormality is quite subtle and impingement is due to the high demands placed on the hip (ballet, hockey, soccer, etc.). Over time, repetitive impingement can cause tearing of the labrum and surface cartilage damage and can subsequently lead to early arthritis.
Labrum Tears
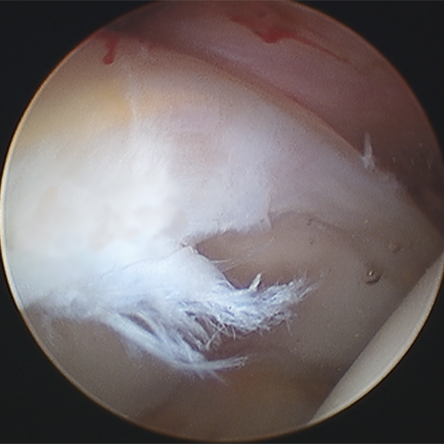
Labral tears most commonly occur due to repetitive injury in the setting of long-standing hip impingement (FAI) or hip instability (dysplasia), but may also occur from a combination of both pathologies as it is common to see dysplasia and FAI at the same time (too much bone of the ball side, not enough on the socket side). Less commonly, a single traumatic event or injury can cause a labral tear. Examples for that are motor vehicle accidents or childbirth. If the labrum becomes torn or detached from the rim of the socket, its function is compromised, and it usually leads to hip pain.
Hip Instability & Dysplasia
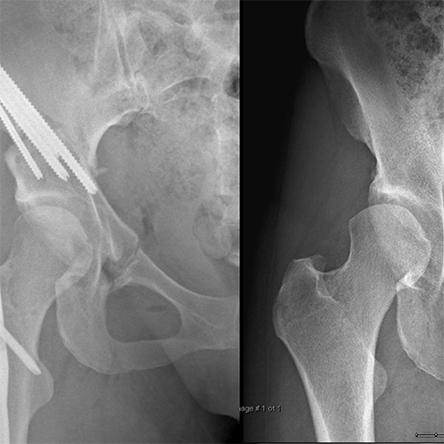
Dysplasia is a congenital disorder in which the hip socket does not cover the ball part of the joint well, leading to poor function of the hip joint. This can be from suboptimal position of the socket, low socket volume, or both, which then gives rise to hip instability, or excessive translational motion and increased shear forces within the joint. Typical anatomic abnormalities in acetabular dysplasia include shallow socket, enlarged labrum, ligamentous laxity or loose ligaments, and/or excessive hip internal rotation or femoral antetorsion.
