Arthritis is defined as chronic joint inflammation and cartilage degeneration. The most common type of arthritis is osteoarthritis, which has a strong genetic component and involves painful and progressive loss of surface cartilage. Other less common forms of arthritis include:
Common Arthritis symptoms include night pain, reduced range of motion, pain in external rotation and pain after prolonged sitting. The hallmarks of osteoarthritis include radiographic signs such as asymmetric cartilage loss, bone spur formation and cyst formation, with other indicators including progressive stiffness and deformity of the joint leading to loss of motion. Arthritis is diagnosed by combining clinical symptoms (pain, stiffness, swelling, deformity) with radiographic (x-ray) findings (joint space loss, bone spur formation, cysts).
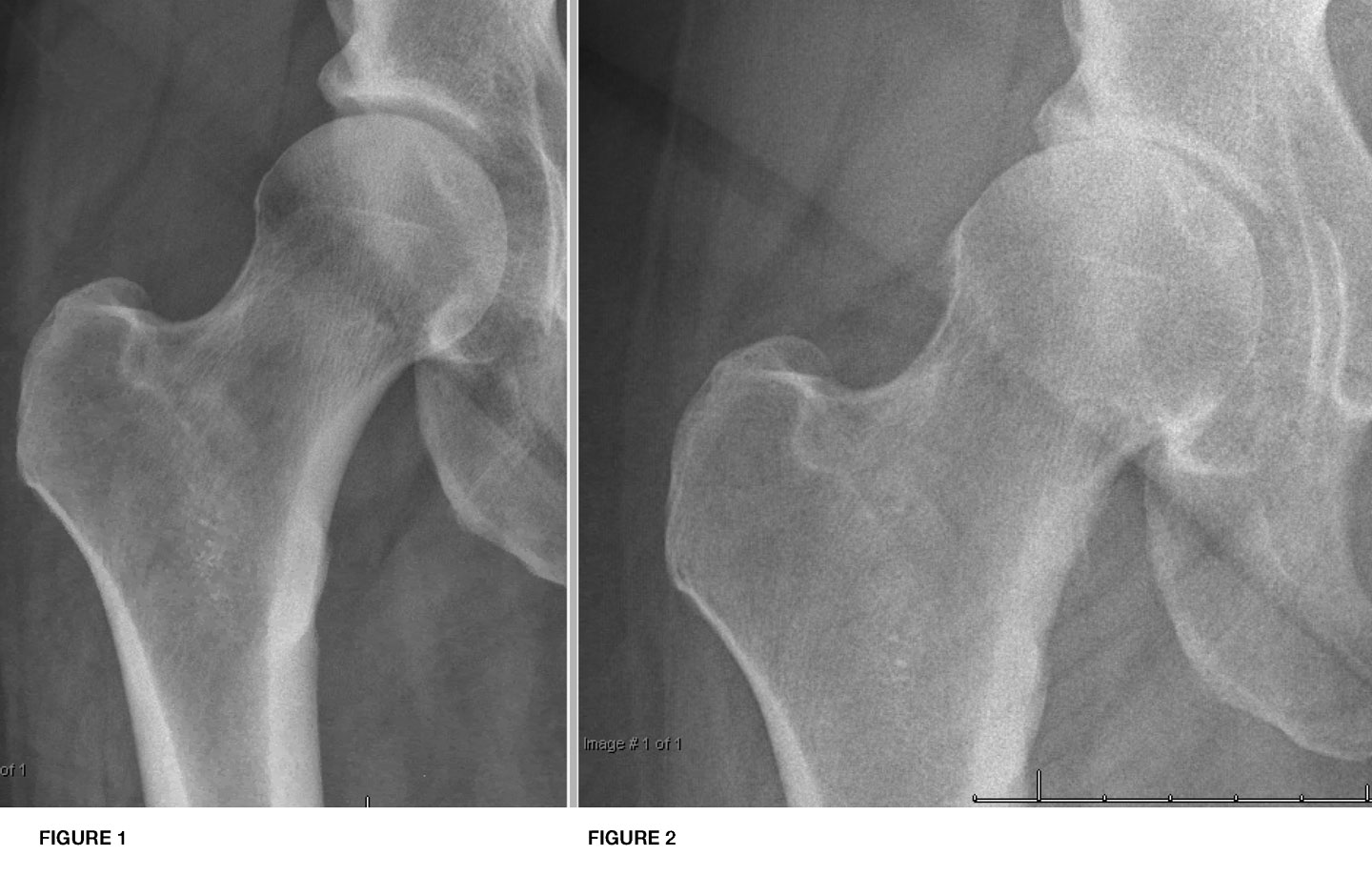
Arthritis is diagnosed by combining clinical symptoms (pain, stiffness, swelling, deformity) with radiographic (x-ray) findings (joint space loss, bone spur formation, cysts). Occasionally, patients will present with radiographic evidence of arthritis and have minimal clinical symptoms. Even if the x-rays show “bone-on-bone” arthritis, the treatment is always guided by the clinical symptoms and not the radiographic findings.
There are many different treatment options for hip arthritis, all of which aim to reduce pain and improve function. Conservative treatment options include:
When these measures fail to provide sufficient pain relief, the next step is to discuss hip replacement surgery. The most reliable way to definitively treat severe hip arthritis is through a hip replacement or hip resurfacing. Postponing THR, if an option, would prevent the need for early life activity modifications and may enable the patient to utilize future and better hip implants that were not yet available before.
Drs. Mei-Dan and Lee and the hip team will help you learn about what these procedures can do for you so you are equipped to make the best decision for your hip joint.